1. I. Introduction
pilepsy is very common disorder or a group of neurological diseases, characterized by seizures [1,2] which take various forms and result from episodic neuronal discharges, the forms of the seizure depending on the part of the brain affected. Epilepsy affects 0.5% of the population. Often there is no recognizable case although it may develop after brain damage, such as trauma, infection or tumor growth or other kind of neurological disease, including various inherited neurological syndromes. Epilepsy is treated mainly with drug through brain surgery may be used for several cases [3,4]. Current antiepileptic drugs are effective in controlling seizures in about 70% of patients [5,6,7]. Anticonvulsants act to prevent the spread of the neuronal excitation by mechanisms that are not fully understood, but which can be roughly divided in to those which involve stabilizing effect on excitable cell membranes, and those which involves enhanced functional activity of neurotransmitters such as gamma amino butyric acid (GABA), which then act to inhibit spread of seizure activity by blocking synaptic transmission at some point. Status epilepticus is potentially fatal, and is a medical emergency requiring swift and effective treatment to minimize the risk of brain damage. [3,5] The term epilepsy refers to a disorder of brain function characterized by the periodic and unpredictable occurrence of seizures. Seizures can be "nonepileptic." When evoked in a normal brain by treatments such as electroshock or chemical consultants or "epileptic" when occurring without evident provocation. [6,8] Epilepsy is a chronic disorder of the Central Nervous System (CNS) with a prevalence rate between 3 and 6 per thousand populations. [8,9] Generalized Seizure: a) Generalized tonic-clonic seizures (GTC, major epilepsy, grand mal) Commonest, lasts 1-2min. the usual sequence is aura, cry and unconsciousness-tonic spasm of all body muscles clonic-jerking followed by prolonged sleep and depression of all CNS functions.
2. II. Types of Epilepsies
3. b) Absence seizures (Minor epilepsy, Petit mal)
Prevalent in children, lasts about ½ min. Momentary loss of consciousness, patient apparently freezes, stares in one direction, no muscular component or little bilateral jerking. EEG shows characteristic 3 cycle per second spike and wave pattern.
4. c) Atonic seizures (A Kinetic epilepsy)
Unconsciousness with relaxation of all muscles due to excessive inhibitory discharges. Patient may fall.
5. d) Myoclonic seizures
Shock-like momentary contraction of muscles of a limb or whole body. Last ½-1min. often secondary. Convulsions are confined to a group of muscles or localized sensory disturbance depending on the area of cortex involved in the seizure, without loss of consciousness. b) Complex partial seizures (CPS, Temporal lobe epilepsy, Psychomotor) Attacks of bizarre and confused behavior and purposeless movements, emotional changes lasting 1-2 min along with impairment of consciousness. An aura often proceeds. The seizure focus is located in the temporal lobe.
6. c) Simple partial or complex partial seizures secondarily generalized
The partial seizure occurs first and evolves in to generalized tonic-clonic seizures with loss of consciousness.
7. IV. Mechanism of Action of Antiseizure Drugs
Order to bring normal balance between excitery and inhibitory postsynaptic potential, antiseizure drugs may use one or more of the following mechanisms.
8. a) Enhancement of GABA-mediated inhibition
The drug may act directly on the GABAreceptor-chloride channel complex (e.g., benzodiazepines, barbiturates) and inhibit the metabolism of GABA (e.g., vigabatrin, valproate) or increase the release of GABA (e.g., gabapentin).This mechanism provides protection against generalized and focal seizures.
9. b) Suppression of rapid repetitive firing
This mechanism of action of antiseizure drugs (Phenytoin, carbamazepine, valproate and lamotrigine). Involves the prolongation and the closing of inactivation gate of Na+ channels, thus reducing the ability of neurons to fire at high frequencies.This mechanism provides protections against maximal electric shock in animals and focal seizures in humans.
10. c) Reduction of current through T-type Ca++ channels
A low threshold Ca++ current (T-type) governs oscillatory response in thalamic neurons. Reduction of this current by antiseizure drugs (e.g, ethosuximide, dimethadione and valproate) explains the mechanism of action against absence seizures. V. Diagonosis [10,11] a
11. ) The electroencephalogram (EEG)
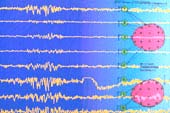
The EEG is central to the diagnosis of epilepsy. To record the brain's electrical rhythms, a number of electrodes (usually 22) are placed against the scalp, arranged in a fixed pattern. They may be held in place by a rubber cap device, or, if longer recordings are required, they can be secured by an adhesive chemical Computerized Tomography (CT) is a procedure which allows the radiologist to study images of the brain, as if the brain could be "sliced". In this way, the brain can be examined to exclude tumors, strokes and other localized abnormalities which may have given rise to seizures.
12. c) MRI Scanning
Introduced in the 1980s, MRI (magnetic resonance imaging) uses a strong magnet instead of xrays to take pictures of the brain. It is one of the best and most precise mechanisms for examining the brain, so it is extremely common for doctors to use MRI for diagnosis in epilepsy. It allows them to look at nerve tissue, the flow of blood and spinal fluid and any tumors or other localized changes or injuries.
13. d) Scanning with Radioisotopes
It is here that radioisotope scanning comes into its own. For this purpose, two types of scanning may be used:
? SPECT (Single Photon Emission Tomography) ? PET (Positron Emission Tomography) Fig. 4 : MRI Scanning
14. VI. General Causes of Epilepsy
The causes of epilepsy are summarized in three general etiological groups.
The first one is the threshold, which determines the susceptibility of individual brains to generate seizures in response to epileptogenic perturbations. This will determine what is called PRIMARY or IDIOPATHIC epilepsy, when it is not the result of some other brain abnormality. They are usually benign and often remit spontaneously or after uninterrupted pharmacological treatment with antiepileptic drugs (AED). The duration between onset and remission can vary from 2 to 12 years.
The second group is related to a specific epileptogenic abnormality, which could be an acquired lesion of the brain, congenital malformations of the brain or genetic disorders other than epilepsy. These SECONDARY or SYMPTOMATIC epilepsies are very common in developing countries, where they are responsible for the difference in terms of prevalence and prognosis. neuromalaria), and these are far more common than in industrialised countries. Their control requires, in addition to AED, specific care of the aetiology (medical and/or neurosurgical).
The third group is represented by epileptic disorders that are probably symptomatic, but the causes have not been identified with existing diagnostic means, and therefore they are called CRYPTOGENIC (which means hidden cause)with a high suspicion of a genetic (but non identifiable) factor.
VII. Treatment [11,12] The goal for individual patients is no seizures and minimal side effects and the job of the physician is to aid the patient to find the best balance between the two during the prescribing of anticonvulsants.
15. Devices:
The vagus nerve stimulator (VNS) is a device that sends electric impulses to the left vagus nerve in the neck via a lead implanted under the skin. It was FDA approved in 1997 as an adjunctive therapy for partialonset epilepsy.
16. Volume XVI Issue I Version I
17. VIII. Surgical Treatment
Epilepsy surgery is an option for patients whose seizures remain resistant to treatment with anticonvulsant medications who also have symptomatic localization-related epilepsy; a focal abnormality that can be located and therefore removed. The goal for these procedures is total control of epileptic seizures although anticonvulsant medications may still be required.
The most common surgeries are the resection of lesions like tumors or arteriovenous malformations which, in the process of treating the underlying lesion, often result in control of epileptic seizures caused by these lesions.
18. IX. Other Treatment a) Ketogenic diet
A high fat, low carbohydrate diet developed in the 1920s, largely forgotten with the advent of effective anticonvulsants, and resurrected in the 1990s. The mechanism of action is unknown. It is used mainly in the treatment of children with severe, medically-intractable epilepsies.
19. b) Electrical stimulation
Methods of anticonvulsant treatment with both currently approved and investigational uses. A currently approved device is vagus nerve stimulation (VNS). Investigational devices include the responsive neurostimulation system and deep brain stimulation.
20. c) Vagus nerve stimulation (VNS)
The VNS (US manufacturer = Cyberonics) consists of a computerized electrical device similar in size, shape and implant location to a heart pacemaker that connects to the vagus nerve in the neck. The device stimulates the vagus nerve at pre-set intervals and intensities of current. Efficacy has been tested in patients with localization-related epilepsies demonstrating that 50% of patients experience a 50% improvement in seizure rate.
Case series have demonstrated similar efficacies in certain generalized epilepsies such as Lennox-Gastaut syndrome. Although success rates are not usually equal to that of epilepsy surgery, it is a reasonable alternative when the patient is reluctant to proceed with any required invasive monitoring, when appropriate pre surgical evaluation fails to uncover the location of epileptic foci, or when there are multiple epileptic foci.
21. d) Responsive neurostimulator system (RNS)
(US manufacturer Neuropace) consists of a computerized electrical device implanted in the skull with electrodes implanted in presumed epileptic foci within the brain. The brain electrodes send EEG signal to the device which contains seizure-detection software. When certain EEG seizure criteria are met, the device delivers a small electrical charge to other electrodes near the epileptic focus and disrupt the seizure. The efficacy of the RNS is under current investigation with the goal of FDA approval. (US manufacturer Medtronic) consists of a computerized electrical device implanted in the chest in a manner similar to the VNS, but electrical stimulation is delivered to deep brain structures through depth electrodes implanted through the skull. In epilepsy, the electrode target is the anterior nucleus of the thalamus. The efficacy of the DBS in localization-related epilepsies is currently under investigation.
22. Volume XVI Issue I Version I

| Category | Drugs | Use |
| Aldehyde | Paraldehyde | Status Epilepsy |
| Aromatic allylic alcohol | Stiripentol | Myoclonic epilepsy |
| Barbiturates | Phenobarbital, | Status Epilepsy |
| Methylphenobarbital, | ||
| Barbexaclone | ||
| Benzodiazepines | Clobazam, | Status Epilepsy |
| Clonazepam, | ||
| Diazepam, | ||
| Midazolam, | ||
| Lorazepam | ||
| Carbamates | Carbamazepine, | Status Epilepsy |
| Oxcarbamazepine | ||
| Fatty acids | Valproic acid, | Absence seizures |
| Divalproex, | ||
| Progabide, | ||
| Tiagabine | ||
| Fructose derivative | Topiramide | Pentylenetetrazol clonic seizures |
| GABA Analogue | Gabapentine, | Simple partial seizures |
| Pregabaline | ||
| Hydantoin | Ethotoin, | Simple and complex partial |
| Phenytoin, | seizures | |
| Mephentoin, | ||
| Fosphenytoin | ||
| Oxazolidinedione | Paramethadione, | Simple partial seizures |
| Trimethadione, | ||
| Ethadione | ||
| Pyrimidinediones | Primidone | Simple partial seizures |
| Succinimide | Phensuccimide | Absence seizures |
| Mesuccimide | ||
| Triazine | Lamotrigine | Generalised tonic-clonic seizures |
| Valproylamides | Valpromide, | Myoclonic and atonic seizures |
| Valnoctamide |
| Year 2016 |