1. Introduction
adelung deformity is a rare wrist malformation consisting of excessive radial and palmar angulation of the distal radius caused by a growth disorder of the palmar and ulnar part of the distal radius physis. This leads to shortening and angulation (recurvatio) of the epiphysis, causing a pathognomonic inclination of articular surface palmarly and ulnarly.
Shortening of the radius may cause the development of progressive incongruency at the DRUJ and a positive ulnar variance. This carries to a dorsal subluxation of the distal ulna, causing the altered aspect of the wrist with the prominent ulna.
Step-by-step alterations of the distal radius and the DRUJ are important contributor factors of the socalled carpus pyramidalization, a progressive increase of carpus convexity, and of the volar carpus subluxation.
Other anomalies described are:
? Vickers ligament or radio-lunate ligament. It is an accessory volar ligament hypertrophic connecting distal radius metaphysis, TFCC, and volar surface of lunate. It is responsible for a compressive injury at the ulnarside of the distal radius physis and a proximal traction of the lunate, determining its collapse between radius and ulna [1][2] . ? Volar radio-triquetral ligament. It may be present dorsally to Vickers ligament. It is characterized by greater dimension and distal insertion to triquetrum [3][4][5] . ? Anomal insertion of pronator quadratus muscle 6 and presence of accessory muscles.
Madelung deformity is a rare condition, the incidence is unknown, and there is no described racial predominance.
Usually, patients come to medical observation between 8 and 14 years old, although there are in literature cases of Madelung deformity at birth or childhood. It is more common in females, the M:F rate of the disorder is 1:4. Madelung deformity can be bilateral about in a third of patients. It may be associated with Léri-Weill dischondrosteosys 7 . There are several types of Madelung deformity 8 :
? Dysplasic type is the more common. It is associated to Léri-Weill dischondrosteosys; Clinically, patients complain of movementrelated pain, altered aspect of the wrist, functional limitations especially in prono-supination.
In literature several therapeutic options are reported [9][10][11] , but because of the limited number of cases, due to low incidence, it is difficult to determine the efficacy of proposed treatment strategies.
? Wait & see for asymptomatic or paucisymptomatic cases; ? Surgery: correction of deformity, release of Vickers ligament and arthrodesis o shortening osteotomy of the ulna.
In the present study, we report our experience in surgical correction of Madelung deformity with the release of Vickers ligament, distal convexity dome osteotomy of the distal radius, and reverse wedge.
2. II.
3. Materials and Methods
Between 2017 and 2019, four patients (2 males and 2 females) affected by Madelung deformity were treated in our clinic.
Three adolescents aged between 12-14 yearsold and a 30-year-old adult. Three patients had a bilateral Madelung deformity with a mild deformity in the untreated limb (tab.1).
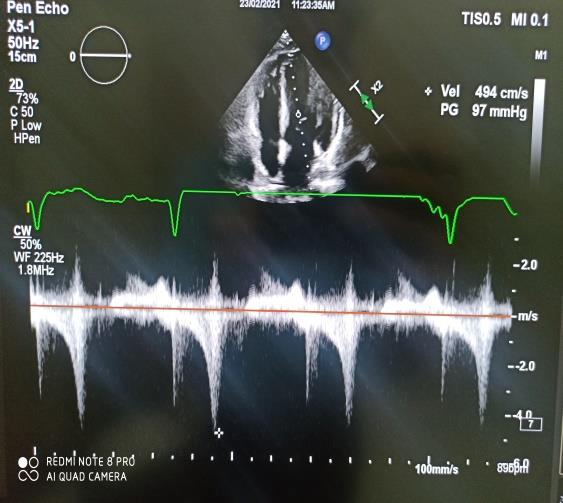
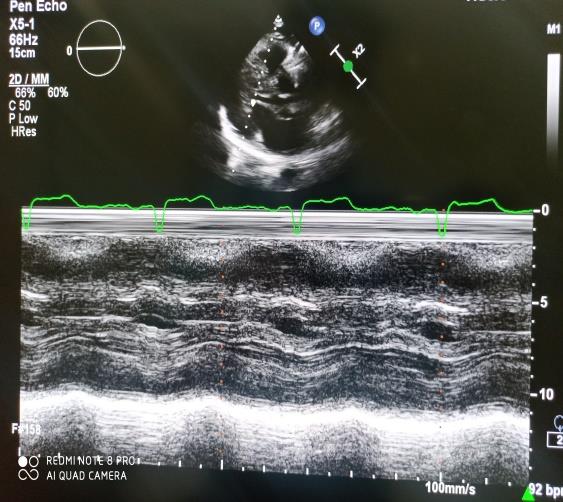
For preoperative planning (fig. 1) we acquired plain radiographs (AP, LL, and oblique projections), MRI to evaluate surrounding soft tissue (in particular presence/absence of Vickers ligament), and CT scans for better analysis of the deformity.
CT scan data were sent to a workstation in standard DICOM format (PACS, Carestream) to create 3D models of the affected wrist. For all patients polyamide templates of the deformed wrists (scale 1:1) were manufactured using a 3D-printer. Harley et al. [12][13] in 2006 and then in 2013 described a surgical correction with dome osteotomy of the distal radius. The technique described provides a dome osteotomy with distal concavity for biplanar Use of 3D-printed polyamide template in preoperative planning allowed to evaluate rotational center of deformity, plan the osteotomy, evaluate needed degrees for triplanar correction, choose implants and simulate preoperatively surgical procedure.
Preoperative planning using 3D virtual planning and 3D-printed templates improves accuracy of surgical correction with dome osteotomy and reduces surgical duration.
It was used a Henry approach, modified according to Orbay, for all the patients in this serie. Release of Vickers ligament in cases where it was present. After identification of rotational center and level of osteotomy, such as preoperative planning, using a piezoelectric saw (piezosurgery), it was possible to improve the accuracy of the osteotomy and the biplanar correction of the deformity with no risk of thermal necrosis.
In 2 cases it was also needed a bone wedge excision of the radial column for better correction of the deformity on the frontal plane. Then the excised bone fragment was used as auto-graft to fill the gap of dome osteotomy (reverse wedge), allowing faster consolidation and improving stability.
Low-profile mouldable plates were used for fixation because of better adaptability rather than anatomical pre-contoured. At least three screws proximal and three distal to osteotomy were used to fix the plate, avoiding physis and DRUJ. In one case it was noted the absence of the pronator quadratus associated with the presence of palmaris profundus muscle. The latter anomaly was already described in literature 14 .
After surgery, immobilization of the wrist for 3 weeks in a thermoplastic splint was applied to all patients. After this period of immobilization, the wrist and forearm rehabilitation protocol were started for about 6 weeks under the supervision of a hand therapist.
Between 8 and 12 months postoperative plates were removed in order to low the incidence of complication such as tendinitis, infections, and loosening.
The mean follow-up duration was 21 months (range 15-28 months). During this period patients were evaluated like proposed by Peymani et al. 15 in his review. Radiographically McCarroll criteria 16 were used to judge correction, we evaluated ROM clinically, grip strength via Jamar dynamometer. DASH questionnaires were administered to evaluate functional outcomes, NRS to quantify subjective pain. Finally, the aesthetic defects were estimated using a section of the Michigan Hand Outcome Questionnaire.
These data were related to collected data before surgery.
4. III.
5. Results
6. Post-operative radiographs, according to
McCarroll criteria, showed a reduction of ulnar tilt, lunate fossa angle, and palmar tilt; whereas no significant difference of palmar carpal displacement was found (Table2). There were significant improvements in functional outcomes after surgical correction as suggested by DASH scores, mean score 13/100. It has to be considered that only the adult patient answered the work-related section of the DASH questionnaire. The MHOQ scores were improved in all patients on average 30/100 (Table 4).
7. Discussion
The purpose of surgical correction in patients affected by Madelung deformity is to relieve pain and improve wrist functions supporting the lunate.
The pain was relieved in all patients, 2 of them were totally pain-free. Analysis of postoperative ROM, grip strength via Jamar dynamometer, and the DASH scores showed good results. Improved MHOQ scores suggested good aesthetic correction.
Corrective dome osteotomy was evaluated on post-operative radiographs, analyzing the degree of correction according to McCarroll criteria. There was a reduction of pathological angles obtaining in some cases a value close to physiological. However, the aim of surgery is not to restore radius but is to improve wrist functions, avoiding lunate collapse. Therefore, it is important that surgery leads to correction of ulnar tilt, lunate fossa angle, and palmar tilt. In our study, we obtained correction of all these parameters.
There was no difference in palmar carpal displacement values between pre and post-surgical correction. PCD measures the palmar-directed displacement of the carpus (represented by the lunate and capitate) relative to the longitudinal axis of the ulna in the lateral view. There was no correction of PCD values because it was not made any surgical correction of the ulna in contrast with the surgical procedure described by Harley et al. The choice not to modify the deviation of the ulnar longitudinal axis surgically was made so as not to interfere with prono-supination movements since patients showed good ROM preoperatively. The range of motion may worsen if we modify the delicate equilibrium made by the gradual dysmorphic growth of articular surfaces aiming tophysiological anatomy that is not present in DRUJ.
Eventual surgical correction of the ulna may be considered at the end of the skeletal growth (predominantly for aesthetic reasons).
Some limits to the McCarrol criteria, since x-ray projections are operator dependent, is to always obtain perfect AP and LL x-ray projections. This limit may be overcome using a preoperative CT scan that are improved with 3D reconstructions and/or MRI.
Compared to other techniques reported in the literature for the surgical correction of Madelung deformities, our technique appeared to be less invasive with shorter recovery time and improved patient's quality of life.
McCarroll and James 17 described a combined technique that includes osteotomies of radius and ulna (very distal radius osteotomy) through a dorsal approach. The same authors highlight an important limitation of the surgical technique in pediatric patients because fixation has to be made very close to the physeal growth plate.
Our technique allows to extend the indications to very young patients because the dome osteotomy and the fixation are made more distant to the physeal growth plate.
Another limit showed by McCarrol and James is the development of a post-surgical DRUJ instability, often asymptomatic. This is another contributing factor for our choice not to correct surgically the ulna. Dome osteotomy showed some common points with cylindrical corrective osteotomy for Madelung deformity proposed by Imai et al. 18 . Both techniques agree to the fundamental use of CT scan and the case report used a dedicated software for the preoperatory planning, for the line of osteotomy, and to create custom-made cutting guides.
Custom-made cutting guide improve surgical accuracy to the preoperative planning, but they limit ulnar column lengthening, using bone wedge excised from radial column osteotomy (reverse wedge).
The use of a pre-op 3D printed model improves surgeons' evaluation and pathology by way of tactile and visual experience 19 . Furthermore, this technology supports the surgeon by selecting the most adequate device for osteosynthesis and helps patients and parents to understand the surgical procedure they will undergo. 20 V.
8. Conclusions
The experience with our patients (even if not statistically significant) showed encouraging results in the use of radial dome osteotomy for the correction of Madelung's deformity.
Our experience suggests that the use of 3D printed bone models in preoperative planning improves accuracy on surgical procedure and on the choice of implants.
In the near future, thanks to a larger sample, our effort will be to standardize this technique as much as possible, providing precise and adaptable indications to each individual case in order to improve the preoperative planning aiming to achieve even better surgical results.
| o Surgical correction of the radius: physiolysis with or | ||||||
| without release of Vickers ligament; opening or | ||||||
| closed wedge osteotomies; reverse wedge | ||||||
| osteotomy; | ||||||
| o Surgical correction of the ulna: epiphysiodesis; | ||||||
| shortening osteotomy, Darrach's technique; | ||||||
| Sauvè-Kapandji technique; | ||||||
| o Combined surgery on radius and ulna; | ||||||
| o Release of Vickers ligament | ||||||
| Pz | Age | Bilateral | Treated limb | Follow-up (months) | Form | Vickers ligament |
| 1 | 3 | yes | right | 15 | Idiopatic | Yes |
| 2 | 12 | yes | right | 26 | Genetic: Léri-Weill | Yes |
| 3 | 13 | yes | left | 16 | Idiopatic | No |
| 4 | 13 | no | right | 28 | Idiopatic | No |
| Pz | UT | LS | LFA | PCD | PT |
| 1 | *48.7° | *21 mm | *50,8° | *27 mm | *27,8° |
| **38° | **9 mm | **33,1° | **27 mm | **18,1° | |
| 2 | *60,3° | *3 mm | *56,6° | *20,5 mm | *21,3° |
| **41,7° | **4,95 mm | **45° | **24 mm | **16,6° | |
| 3 | *45° | *6,82 mm | *48,3° | *22 mm | *52,6° |
| **31° | **6,63 mm | **33,9° | **22 mm | **41,1° | |
| 4 | *43,6° | *12 mm | *51,3° | *31 mm | *21,5° |
| **41° | **6 mm | **47à° | **27mm | **17,4° | |
| UT = ulnar tilt; LS = lunate subsidence; LFA = lunate fossa angle; PCD = palmar Carpal displacement; | |||||
| PT = palmar tilt. | |||||
| Pz | Grip strength | Pain (NRS) | F | E | Range of motion UD RD | S | P |
| Pz | DASH | MHOQ |
| 1 | *19,4/100 | *50/100 |
| **11,1/100 | **75/100 | |
| 2 | *51,62/100 | *62,5/100 |
| **45/100 | **50/100 | |
| 3 | *22,4/100 | *68,75/100 |
| **7,76/100 | **93,75/100 | |
| 4 | *34,17/100 | *18,75/100 |
| **11,16/100 | **43,75/100 | |
| IV. |