1. Introduction
. pneumoniae, described by Edwin Klebs in 1875, is a gram-negative bacterium belonging to the Enterobacteriaceae family. It caused severe infections in critically ill patients, newborns, immunocompromised individuals or those with other risk factors in healthcare establishments [1,3]. Carbapenemresistant Klebsiella pneumoniae (CRKP) has emerged as a major nosocomial pathogen worldwide and constitutes a significant growing public health threat in developing and developed countries due to the indiscriminate consumption of carbapenem antibiotics that has accelerated the incidence of antibiotic resistance in recent years [1,5,10]. Carbapenem resistance is typically mediated by the production of carbapenem-hydrolyzing enzyme through the evolution of high-risk clones by acquiring, retaining, and efficiently transmitting resistance genes, and unrestricted consumption promoted the rising trend as well. Carbapenem-resistant Enterobacteriaceae were first described in the early 1990s, and the isolation of carbapenem resistant K. pneumoniae strains occurred sporadically throughout that decade [11]. Over the past few years, however, the recovery of carbapenemresistant Klebsiella pneumoniae strains from diverse clinical specimens has increased at an alarming rate because carbapenems are widely used to treat infections, especially those caused by Enterobacteriaceae, a producer of extended-spectrum ?-lactamase (ESBL).
CRKP bloodstream infections are associated with higher mortality than other infection types of CRKP and require treatments timely, especially in hematological patients. This study was used to establish a risk prediction model of CRKP in this region and seek appropriate treatment in this population. Bloodstream infections caused by CRKP increase the rate of treatment failure and death. Recent estimates suggest that attributable mortality may be as high as 44%, particularly in the setting of bacteremia, with total economic costs exceeding $553 million annually in the United States based on current incidence [1].Previous studies have found a crude mortality rate ranging from 44% to 33% for diverse infections caused by carbapenem-resistant K. pneumonia [5,12]. In our region, where K. Pneumoniae represented 18% of all urinary Enterobacterales isolates and the second leading cause of health care-associated UTIs, and CRKP is increasingly implicated that accounts for 42.5% of all urinary K. pneumoniae isolates. In line with our study, Patients in the ICU are at a risk of infections caused by carbapenem-resistant K. pneumoniae, which is emerging as a risk to causes various nosocomial infections, notably 40% in respiratory tract infections, 59-60% of body fluids and pus samples. Therefore, we set out this study to determine the prevalence of carbapenem resistance among clinical K. pneumoniae isolates originated from different sections of the hospitals, which affiliated with our lab and walk-in lab in Delhi, northern region of India.
2. II.
3. Material and Methods
This retrospective study was performed in the Microbiology department of Dr. Lal Path Labs in Delhi, North India. A total of 3662 K. pneumoniae isolates recovered from diverse samples were correctly identified using a matrix-assisted laser desorption ionization timeof-flight mass spectrometry (MALDI-TOF MS, Bruker Daltonics, Bremen, Germany).
Antibiotic susceptibility testing done by VITEK-2 (Biomerieux) system from the pure culture of isolated colonies of the Klebsiella pneumonia on Bloodagar; the Gram-negative bacteria were inoculated on to N405 card, and the breakpoint (susceptible, intermediate, or resistant) was interpreted according to Enterobacterales M100-S31provided by the Clinical and Laboratory Standards Institute (CLSI) standards. The antibiotic susceptibility tests were conducted for Ampicillin, Amoxicillin clavulanic acid, Piperacillin-tazobactam, Ciprofloxacin, Levofloxacin, Cefuroxime, Ceftriaxone, Cefepime, Cefoperazone/sulbactam, Amikacin, Gentamicin, Trimethoprim-sulfamethoxazole, Ertapenem, Meropenem, Imipenem, Fosfomycin, and Nitrofurantoin. All ASTs, except Tigecycline, were interpreted according to the criteria of Enterobacterales in the Clinical and Laboratory Standard Institute (CLSI) guideline (2021) [15]. The interpretation of Tigecycline followed the European Committee on Antimicrobial Susceptibility Testing (EUCAST) (2021). However, Colistin was recommended to treat CRKP infection by EUCAST. Thus, Colistin susceptibility was not routinely tested or included in our study because of its severe side effects such as nephrotoxicity, neuromuscular blockade.
In this study, Minimum inhibitory concentration (MIC) breakpoints were used as a testing method that have to detected carbapenem-resistance, and this test can be carried out using broth micro dilutions by automated antimicrobial susceptibility testing (AST) systems (VITEK-2). CRKP was defined as isolated Klebsiella pneumoniae strains resistant to carbapenem agents, including ertapenem, meropenem, or imipenem. Klebsiella pneumoniae isolates are associated with a suspicion of carbapenemase production based on updated carbapenem breakpoints (imipenem or meropenem or ertapenem MICs according to breakpoints defined by the CLSI at least ?2µg/mL). ATCC700603 was used as the quality control strain for the antibiotic susceptibility tests. To avoid duplicate counts, only the first strain was included for every patient, based on the ID number.
4. Statistical Analysis:
The analysis was done using the Statistical Module of Myla Application from bioMerieux. Age, gender, antibiotic sensitivity and resistance with MIC were included as variables in this study. Myla is a browser-based application that consolidates and covers the microbiology data into actionable information. The Statistical Reporting Module is a specific MYLA(r) computer application which allows to Manage, Configure and generate different types of Microbiology Statistical Report in few clicks." III.
5. Results
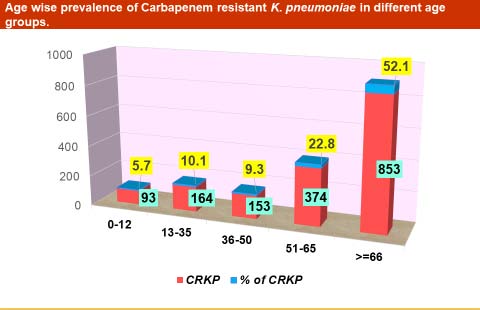
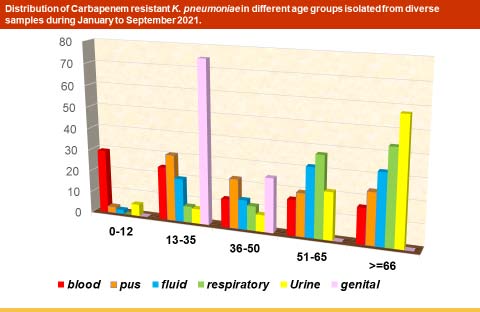
Of the total 3662 isolates of Klebsiella pneumonia from the diverse clinical specimens, 1637 isolates (44.7%) were confirmed to be 100% carbapenem-resistant, in which the highest occurrence of CRKP was found in blood samples comprising (67.1%) followed by Pus (61.2%), Body fluids (59.4%), Urine (42.7%), Respiratory (41.9%) and genital vaginal (13.8%) respectively (Table 1). Among the total 1637 CRKP isolates, 923 (56.4%) were isolated from males, while the remaining 714 (43.6%) were from females. Among these CRKP strains, 75% of patients were generally elderly (with a range of 51 to >65 years), followed by younger adults (10.1%), adults (9.3%) and children (5.7%), respectively (Figure 1). In our study, it appeared that Tigecycline was still the good choice of CRKP, with susceptibility (57%) Other options might be amikacin (54%) and TM/SXT (42%) and their MIC values were as follows: Tigecycline (57%; MIC 50/90 0.5/8 ug/ml), Amikacin (54%; MIC 50/90 4/64 ug/ml), TM/SXT (42%; MIC 50/90 40/320ug/ml) and Fosfomycin (71%; MIC 50/90 16/256ug/ml). However, the susceptibility to these antibiotics was only slightly higher than 50%. While other antibiotics sensitive pattern, which were tested against CRKP isolates, was as follows: Amoxicillin/clavulanic acid (23%), Ceftriaxone (6%), Cefuroxime (4%), and Ciprofloxacin (12%). In recent years, Fosfomycin (susceptibility of 71%) has been recommending as a supplement in treating CRKP infection, although the CLSI standards propose it only for the treatment of urinary tract infections. The antibiogram and MIC results of the CSKP and CRKP isolates for all tested drugs are given in Table 5. Among IV.
6. Discussion
However, Urinary tract infections (UTIs) are the most common infections in India. For the first time in our region, where the emergence of carbapenem-resistant K. pneumoniae strains was noted that accounted for 42% of all the urinary K. pneumoniae isolates. In addition, particularly noteworthy findings that isolation of CRKP from the urine was most commonly associated UTIs in higher age group, which is inconsistent with other findings [4,[6][7]. Taken together, these findings provides new insights into the clinical demonstration of CRKP bacteriuria and are useful for drawing up management strategies against XDR pathogens. Our huge sample made it possible for us to draw definitive conclusions for CRKP in UTIs; Fosfomycin71% sensitive may be a viable option for treating CRKP in Delhi if the organism tests as susceptibleand we found a growing prevalence of CRKP in the UTIs through retrospective analysis, consistent with findings from previous large surveillance studies [7].
Our data showed that constantly use or misuse of carbapenems evolving Carbapenem resistance K. pneumoniae is the main contributing factor for XDR and usually, the definitive step before pan drug resistance (PDR) which were worrying and is dramatically limiting treatment options [13,14]. Therefore, older agents, such as polymyxins and fosfomycin, which were rarely implemented in the past because of efficacy and toxicity concerns, together with the newer tigecycline, have become last-resort choices.
The CRKP isolates are usually XDR and are susceptible only to Tigecycline and one or more aminoglycosides. Recently, our study showed that Tigecycline, Amikacin, and TM/SXT appear to be suitable therapies for slightly higher than 50% of the bloodstream and other infections caused by carbapenem-resistant Klebsiella pneumonia, which draws attention to Tigecycline resistance, and this finding is similar to other studies [10,[13][14].This is in contrast to other studies where Tigecycline had good activity against CRKP (95.5%) [2,8,12]. In this study, it appeared that only Tigecycline could be a good choice (susceptibility of 57%); at the same time, TM/SXT and amikacin might be an alternative, its susceptibility was only slightly higher than 40% and 50%, respectively. These findings indicate that the resistance rate of CRKP varies among different countries and period to period, even in the same country that may be explained in part by different levels of antibiotic use.
Therefore, we concluded that combination therapy including high-dose meropenem, fosfomycin, tigecycline and aminoglycosides are widely used, with suboptimal results is often required in the management of CRKP infections. Although there has been a need for rapid development of new antibiotics, such as ceftazidime-avibactam, and more effective counteractive measures, such as antimicrobial scientific stewardship and improved hospital infection control procedures, 1637 CRKP isolates, 36(2.2%) isolates were resistant to all tested antibiotics (pan drug-resistant); these isolates did not respond to the last-resort antimicrobial Tigecycline.
Our study reported that carbapenem-resistant K. pneumoniae was the strongest predictor of bloodstream infection among all the clinical samples studied Blood contained the highest percentage of CRKP, and this finding was also consistent with a study done in south India [10], but we have no data of mortality rates associated with severe sepsis and septic shock. Whereas other studies reported, the crude mortality rate of up to 44% attributable to carbapenemresistant K. pneumonia bacteremia is the highest so far for any microorganism causing bacteremia [3]. However, other studies determined the high ratio of CRKP isolated from urine [4,6,7], sputum [2,5], pus [8], respectively. In addition, the present study investigated 61% of CRKP strains were reported from different pus sites. In contrast our neighbor country reported wound samples (49.4%) were the source of the CRKP infection that were significantly associated with the general surgery ward. This study is retrospective and has some limitations, difficult to explain, such as the length of stay and time of collection of diverse samples, which could not be ascertained.
Klebsiella pneumoniae is among one of the most commonly detected multidrug-resistant member of the Enterobacterales family emergence of carbapenem resistant Klebsiella pneumonia (CRKP) has resulted in limited effective treatment strategies, posing a healthcare threat worldwide [1][2][3][4][5][6][7][8][9][10]. The global prevalence of carbapenem-resistant Klebsiella pneumoniae has become alarming especially in developing and developed countries with inconsistent antibiotic policies. To our knowledge, this was the first study to focus on the burden and susceptibility of carbapenem-resistant K. pneumonia (CRKP) in diverse samples present alarming in north India that emphasizes contributing factor to extensive drug resistance, and their recent acquisition and dissemination likely predicted pan-drug resistance shortly. However, blood, urine, sputum, tracheal secretion and pus were the major source of CRKP worldwide, which is similar to our findings [2,[4][5][6][8][9][10].
Our results present a worrying trend of CRKP 44.7% among K. Pneumoniae isolates, which is similar to the previous study where Egyptian literature showed a prevalence of 44.3% of CRKP isolates [2,5]. Similarly, other studies showed varying prevalence rates from 20 to 60% in India and other countries [3,5 7-9]. In our study, the CRKP was found to be highest in elderly patients ranging 51 to>=66 which is similar to the other studies [2,[4][5][6] have taken. These data highlight the need for regular surveillance of microbial resistance in India to improve infection control and guide for the use of antimicrobial agents. Newer BL/BLI (Beta-lactam and Beta-lactam inhibitors) are beyond the scope of this study.
V.
7. Conclusion
Our findings concluded that the CRKP existed in north India among diverse isolates that can also be associated with the presence in a high-risk because we are sitting on a time bomb of XDR and PDR bacterial infections; if we do not take necessary steps like antibiotic stewardship in time, then we have limited or no options for treatment. Therefore, the importance of continuous monitoring of carbapenems that emphasizes the urgent need for improved infection control, antibiotic stewardship programs, and utilization of a surveillance and prevention system necessary to prevent the national and transnational spread of these isolates, especially in the case when the healthcare facilities are inadequate. Ethical Approval: It is not applicable.
8. Conflicts of Interest:
There are no conflicts of interest.
| Samples | Total K. pneumoniae isolates N=3662 | Carbapenem resistant K. pneumonia (CRKP) isolates N=1637 (44.7%) |
| Blood | 91 | 61 (67.1%) |
| Pus | 165 | 101 (61.2%) |
| Body fluids | 185 | 110 (59.4%) |
| Respiratory | 191 | 80 (41.9%) |
| Genital vaginal | 29 | 4 (13.8%) |
| Urine | 3001 | 1281(42.7%) |
| Age Specimens | 0-12 | 13-35 | 36-50 | 51-65 | >=66 |
| Blood (n=61) | 18 (29.5) | 15 (24.6) | 8 (13.1) | 10 (16.4) | 10 (16.4) |
| Pus (n=101) | 3 (2.9) | 31 (30.7) | 23 (22.8) | 20 (19.8) | 24 (23.8) |
| Body Fluids (110) | 2 (1.8) | 22 (20) | 15 (13.6) | 35 (31.8) | 36 (32.7) |
| Respiratory (80) | 0 | 6 (7.5) | 9 (11.3) | 30 (37.5) | 35 (43.8) |
| Urine (1281) | 70 (5.4) | 87 (6.8) | 98 (7.7) | 278 (21.7) | 748 (57.7) |
| Genital (4) | 0 | 3 (75) | 0 | 1 (25) | 0 |
| Total No. Antibiotics | Range | CSKP N=2025 (55.3%) Sensitive% R% | CSKP MIC (?g/ml) 50/90 | |
| Ertapenem | ? 0.5 -? 2 | 97.9% | 2.1% | 0.5/0.5 |
| Meropenem | ? 1 -? 4 | 97.2% | 2.8% | <=0.25/0.25 |
| Imepenem | ? 1 -? 4 | 97.6% | 2.4% | <=0.25/0.5 |
| Total No. Antibiotics | Range | CRKPN=1637 (44.7%) Sensitive% R% | CRKP MIC (?g/ml) 50/90 | |
| Ertapenem | ? 0.5 -? 2 | 0% | 100 | 8/8 |
| Meropenem | ? 1 -? 4 | 0% | 100 | 4/16 |
| Imepenem | ? 1 -? 4 | 0% | 100 | 4/16 |
| In this study, K. Pneumoniae isolates originated | Ertapenem (0%; MIC 50/90 8ug/ml), Meropenemand | |||||
| from different sections of the hospitals, which are | Imipenem (0%; MIC 50/90 4-to16ug/ml) respectively. | |||||
| affiliated with our lab and walk in the lab. This study | Whereas 2025 (55.3%) recognized as Carbapenem | |||||
| uses current breakpoints recommended by CLSI (M100- | Sensitive Klebsiella pneumoniae (CSKP) were | |||||
| S31) for carbapenem interpretation, 1637 (44.7%) out of | susceptible to carbapenem97%and MIC values of the | |||||
| 3662 K. pneumoniae isolates were nonsusceptible | tested ?-lactam antibiotics were as follows: MIC 50/90 | |||||
| (intermediate and resistant) to Ertapenem, Meropenem | 0.5ug/ml for Ertapenem, MIC 50/90 <=0.25 to 0.5ug/ml for | |||||
| and Imipenem recognized as Carbapenem-Resistant | Meropenem, and Imipenem respectively in all tested | |||||
| Klebsiella pneumonia (CRKP). Susceptibility pattern and | strains [Table 3, 4]. | |||||
| their MIC value of CRKP isolates was as follows: | ||||||
| ORGANISM ANTIBIOTICS | Range | CSKP N=2025 (S%) | CSKPMIC (?g/ml) 50/90 | CRKP N=1637 (S%) | CRKPMIC (?g/ml) 50/90 | |
| Ampicillin | ? 8 -? 32 | 0.9 | 32/32 | 0 | 32/32 | |
| Amoxycillin/clavulanic acid | ? 8 -? 32 | 75% | <=2/32 | 23% | 32/32 | |
| Piperacillin/tazobactam | ? 16 -? 128 | 92% | <=4/16 | 34% | 128/128 | |
| Cefuroxime | ? 4 -? 32 | 76% | 2/64 | 4% | 64/64 | |
| Cefuroxime/Axetil | ? 4 -? 32 | 73% | 2/64 | 3% | 64/64 | |
| Ceftriaxone | ? 1 -? 4 | 95% | 1/1 | 6% | 64/64 | |
| Cefoperazone/sulbatam | ? 16 -? 64 | 97% | <=8/<=8 | 43% | 64/64 | |
| Cefepime | ? 2 -? 16 | 96% | 1/1 | 35% | 32/64 | |
| Amikacin | ? 16 -? 64 | 97% | <=2/2 | 54% | 4/64 | |
| Gentamicin | ? 4 -? 16 | 96% | <=1/<=1 | 47% | 8/16 | |
| Ciprofloxacin | ? 0.25 -? 1 | 62% | 0.5/2 | 12% | 4/4 | |
| Tigecycline | ? 0.5 -? 2 | 86% | <=0.5/2 | 57% | 0.5/8 | |
| Trimethoprim/sulfamethoxazole | ?20 -? 80 | 91% | <=20/40 | 42% | 40/320 | |
| Fosfomycin | ? 64 -?256 | 94% | <=16/64 | 71% | <=16/256 | |
| Nitrofurantoin | ? 32 -?128 | 46% | 64/128 | 16% | 256/512 | |