1. I.
background ver the last few decades, there has been a progressive increase in the rate of cesarean section deliveries in our country. WHO has recommended that this rate should be between 10%and 15% but the driver behind this trend is not completely understood especially in developing countries. 1,2 Immediate and long-term complications of CS included increased risk of maternal mortality and morbidity, increased need for blood transfusion, longer hospitaliz-ation, postpartum infections, retained placenta, stillbirths, postpartum hemorrhage.
Over the last few decades, there has been a progressive increase in the rate of cesarean section deliveries in our country. WHO has recommended that this rate should be between 10%and 15% but the driver behind this trend is not completely understood especially in developing countries. (1,2). The rising cesarean section trend is a major public health concern due to potential maternal and perinatal risks associated with this. Immediate and long-term complications of CS included increased risk of maternal mortality and morbidity, increased need for blood transfusion, longer hospitalization, postpartum infections, retained placenta, stillbirths, postpartum hemorrhage.
To understand this and to implement effective measures to reduce cesarean section rates, a tool is required to monitor and compare cesarean section rates in the same setting over time and among different settings. Traditionally, at the facility level, we monitor cesarean section rates using the overall percentage of deliveries by cesarean section. But because of some intrinsic differences in hospital factors and infrastructure, a difference in characteristics of the population, and differences in clinical management protocols, this "overall cesarean section rate" becomes difficult to interpret and compare. Ideally, there should be a classification system to monitor and compare cesarean section rates. Such a system should be simple, clinically relevant, accountable, replicable, and verifiable (3,4.5). In 2015, WHO introduced Robson's criteria in the year 2015 as a standardized method to determine the rate and indications of cesarean section and issued an implementation manual(6). ? Obstetric history (parity and previous cesarean section) ? The onset of labor (spontaneous, induced, or cesarean section before the onset of labor) ? Fetal presentation or lie(cephalic, breech, or transverse) ? Number of neonates ? Gestational age (pretermorterm). Nulliparous women with a single cephalic pregnancy, ?37 weeks gestation in spontaneous labor 2 Nulliparous women with a single cephalic pregnancy, ?37 weeks gestation who had labor induced or were delivered by cesarean section before labor 2a Cesarean section performed after induction of labor 2b Cesarean section performed before onset of labor 3
2. O
Multiparous women without a previous cesarean section, with a single cephalic pregnancy, ?37 wee ks gestation in spontaneous labor 4 Multiparous women without a previous cesarean section, with a single cephalic pregnancy, ?37 weeks gestation who had labor induced or were delivered by cesarean before labor 4a Cesarean sections performed after induction of labor 4b Cesarean sections performed before onset of labor 5
All multiparous women with one or more previous cesarean sections, with a single cephalic pregnancy, ?37 weeks gestation 5.1 With one previous cesarean section 5.2 With two or more previous cesarean sections 6
All nulliparous women with a single breech pregnancy 7 All multiparous women with a single breech pregnancy including women with previous cesarean section 8 All women with multiple pregnancies including women with previous cesarean section 9
All women with a single pregnancy with a transverse or oblique lie, including women with previous cesarean section 10
All women with a single cephalic pregnancy < 37 weeks gestation, including women with previous cesarean section II.
3. Materials and Methods
This study is a cross-sectional study of 5744 women delivered in the department of obstetrics of S.N. Medical College, Agra performed from 1 st April 2020 to 31 st March 2021. S.N.Medical College is a tertiary referral hospital where around 6000 deliveries take place annually.
All women who underwent cesarean section in the hospital during the specified period were included in the study.
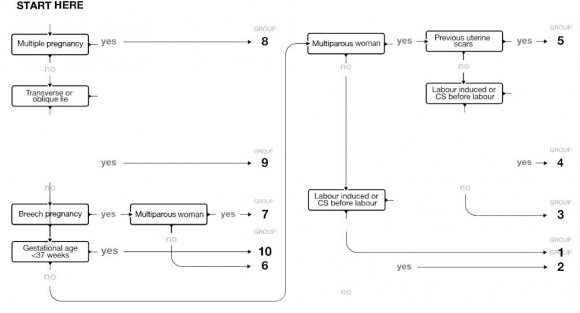
Cases with incomplete information, doubtful gestational age, and laparotomy for uterine rupture were excluded from the study. The identity of women who underwent cesarean section was obtained from the delivery register, admission and discharge register, and operation register. The admission and discharge register and delivery register contained information about all women who delivered in the hospital regardless of the mode of delivery (vaginal, Caesarean section) while the operation register contained only information about women who underwent Caesarean section. Using the medical registration number of each woman, we accessed all Caesarean section files performed during the study.10 groups and their characteristics are shown in table 1. Gestational age was categorized as a term (>/=37 weeks) or preterm (<37 weeks). Patient's demographic data, patient's parity, obstetric history, the onset of labor, fetal presentation or lie, number of neonates, gestational age were collected. The indications for cesarean section were grouped using a flowchart (figure 1).
4. Result
To make the most of the information provided by the Robson Classification in local settings and to allow comparisons between settings, the data is best reported in a standardized way (the "Robson Classification Report Table ") 7 12.9% Can be higher in tertiary hospitals as women with high-risk factors are being referred to our hospital. These women require induction of labor, so it is accompanied by a high rate of cesarean section in this group.
5. Look at the Ratio of the size of Group1 versus Group2
It is usually 2:1 or higher It is always higher than the ratio of Group1/Group2 in the same institution. This is a very reliable finding in confirming data quality and culture of the organization.
6. 5.2
The Ratio of group3:group4 is larger than the ratio of group 1:group2 which strongly signifies the reliability of data 9. Look at the Ratio of the size of Group 6 and Group7.
The ratio of nulliparous breech/multiparous breech is usually 2:1 because breeches are more frequent in nulliparous women than in multiparous women. Ratio 0.94 It can be because of an unusual nullipara/multipara ratio.
C. Steps to assess the rate of cesarean section Table 5: Steps to assess cesarean section rates using the Robson Report Table
7. Steps
Robson guideline Result Interpretation
1. Look at the CS rate for Group1
Rates under 10% are achievable 12.23% It is slightly higher in our hospital.
8. Look at the CS rate for Group2
Consistently around 20-35%
33.83% It is within the appropriate range.
9. Look at the CS rate for Group3
Normally, no higher than 3.0%.
10. 3.57%
Slightly higher than 3%
4. Look at the CS rate for Group 4 It rarely should be higher than15%
22.39% CS rates in Group 4 reflect the size and rates in 4a and 4b. If the size of Group4 is large (there are more cases of prelabour cesarean sections), the overall CS rate in Group 4 is also to be high.
11. Look at the CS rate
for Group 5
Rates of 50-60% are considered appropriate.
12. 69.07%
Rates are higher, this is due to a large number of women with 2 or more previous CS.
13. Look at the CS rate for Group8
It is usually around 60%.
14. 38.02%
The lower rate can be due to more number of multiparous twins or due to nulliparous/multiparous with or without a previous scar.
15. Look at the CS rate in Group10
In most populations, it is usually around 30%
16. Discussion
Cesarean sections are becoming more common over the world, with rates rising from 12% in 2000 to 21% in 2015. 8 In India, the caesarean section rate has been steadily growing from 8.5 percent in 2005-2006 to 17.2 percent in 2015-2016, following global trends. 9 Many authors have expressed their satisfaction with this classification and have suggested that it be utilised more widely. 10,11 Madhav Prasad wrote in a 2015 article that now is an ideal moment for India to use the 10-group Robsons classification to rate caesarean sections. 12 The bulk of caesarean sections were found in groups 2 and 5, according to Deepika Jamwal et al. Group 5 was responsible for 40.3 percent of all caesarean sections, while group 2 was responsible for 29.2%. 13 At a study conducted in a private tertiary care centre in northwest India, Priyanka D. Jogia et al. discovered that group 5 (women with a history of CS) contributed the most (37 percent) to overall surgical deliveries, with group 2 being the second highest contributor (21 percent). 14 Pratima et al conducted a study of 81,784 deliveries (62,336 vaginal and 19,448 Cesarean deliveries) over 3 years. The year-wise CS rate was 22.4%, 23.5% and 25.5%, respectively. The largest contributor was by group 5 followed by group 2 and group 1. Based on 3-year data, it was predicted in the study that the CS rate will increase by 0.905% annually in the coming 3 years. (15). During the study period, our institution's overall caesarean section rate was 26.22 percent, which looks to be higher than the national norm. Robson group 5 was the most significant single contribution to our institution's CS rate. Cesarean section rate in group 1 was higher than recommended i.e.12.23% (rate <10% are achievable) and in group 3 CS rate was 3.57% against the recommended rate of <3%. In group 5 the cesarean section rate between 50-60% is recommended but in our institution CS rate in group 5 was 69% as a large number of women with previous 2 or more cesarean sections were being admitted. The absolute contribution of group 5 is very high (40%), this indicates high CS rates. The size of group 5 is frequently connected to the overall caesarean section rate. The size of group 5 in our study was 15%, which explains our institution's overall increased caesarean section rate. It's also worth noting that Robson group 10 has grown in size (preterm deliveries). Because women with high-risk conditions are referred to our hospital, Robson group 5 can be greater in tertiary hospitals. Induction of labour is necessary for these women, hence there is a high rate of caesarean section in this group. n group 1 and group 2 in previous years.
17. V.
18. Conclusion
Reducing the primary cesarean section rate in group 1 and group 2 will reduce the overall cesarean section rate in the institution.
19. Bibliography
| Group | Number of CS in group | Number women in the group | Group Size1 (%) | Group CS rate2 (%) | Absolute group contribution to overall CS rate3 (%) | The relative contribution of a group to overall CS rate4 (%) |
| 1 | 214 | 1750 | 30.43 | 12.23 | 3.73 | 14.21 |
| 2 | 204 | 603 | 10.49 | 33.83 | 3.55 | 13.55 |
| 3 | 48 | 1346 | 23.43 | 3.57 | 0.84 | 3.19 |
| 4 | 58 | 259 | 4.51 | 22.39 | 1.01 | 3.85 |
| 5 | 603 | 873 | 15.12 | 69.07 | 10.50 | 40.04 |
| 6 | 60 | 77 | 1.34 | 77.92 | 1.04 | 3.98 |
| 7 | 36 | 82 | 1.43 | 43.90 | 0.63 | 2.39 |
| 8 | 27 | 71 | 1.24 | 38.02 | 0.47 | 1.79 |
| 9 | 39 | 42 | 0.73 | 92.86 | 0.68 | 2.59 |
| 10 | 217 | 741 | 12.90 | 29.28 | 3.78 | 14.41 |
| Total* | Total number CS 1506 | Total number women delivered 5744 | 100% | Overall CS rate 26.22% | Overall CS rate 26.22% | 100% |
| Steps | Robson guideline | Result | Interpretation | ||
| 1. The total number of cesarean | These numbers should be the | 57 | We excluded the cases with | ||
| sections and women delivered in our | same as the total number of | incomplete data | |||
| hospital | cesarean sections performed and | ||||
| of women delivered in the hospital. | |||||
| 2. Look at the size of Group 9 i.e. all | It should be less than 1%. | 0.73% It is less than 1% | |||
| women with single ton transverse or | |||||
| oblique lie. | |||||
| 3. Look at the CS rate of Group 9 | It should be 100% by convention. | 92.86 3 | extremely | preterm | |
| pregnancies with intrauterine | |||||
| death of fetus were delivered | |||||
| vaginally | |||||
| B. Steps to assess the type of population | |||||
| Steps | Robson guideline | Result | Interpretation | |||
| 1. Look at the of Group1+ | This usually represents | 40.9% | It is within the acceptable range | |||
| 2i.e. All nulliparous women | 35-42% of the obstetric | |||||
| ?37 weeks gestationsing | population | of | most | |||
| letoncephalic | hospitals. | |||||
| 2. Look at the size of Groups | This usually represents | 26.2% The reason for low size of Groups 3 and 4 | ||||
| 3+4 i.e. All multiparous | about 30% of women. | could be that the size of Group 5 is very high | ||||
| women | ?37 | weeks | which is accompanied by a high overall CS | |||
| gestation | single | ton | rate. | |||
| cephalic, without previous | ||||||
| CS | ||||||
| 3. Look at the size of Group 5. | It is related to the overall | 15.12% Overall CS rate is usually related to the size of | ||||
| (Multiparous women with | CS rate. Group 5 usually | group 5 and the size of this group is larger | ||||
| previous cesarean section | contributes to about half | (>15%) if the institute has high CS rate in the | ||||
| ?37 weeks gestation with | of the total CS rate. In | pasty ears mainly in Groups 1and 2. | ||||
| singleton | cephalic | settings with low overall | ||||
| pregnancy). | CS rates it is usually | |||||
| under10%. | ||||||
| 4. Look at the size of | It should be 3-4% | 2.77% | It is within the acceptable range | |||
| Groups6+7ie. Breeches in | ||||||
| nulliparous | women | + | ||||
| breeches in multiparous | ||||||
| women | ||||||
| 5. Look at the size of Groups 8 | It should be 1.5 -2% | 1.43% | It is nearly within the acceptable range | |||
| Multiples | ||||||
| 6. Look at the size of Groups | It should be less than | |||||
| 10 Preterm cephalic and | 5% in most normal risk | |||||
| singletons | settings. | |||||