1. Introduction
anglioneuromas are benign neurogenic tumors that arise from sympathetic ganglions and are most commonly found in teenagers and young adults. They are usually asymptomatic and sometimes diagnosed by chance. The procedure of choice is Surgical removal. However, it has been proposed that the risks and consequences of this method may outweigh the advantages.
2. II.
3. Case Presentation
A forty-year-old lady presented with cough and expectoration for the last three months. No other constitutional symptoms were present. There was no history of lung cancer among family members. Vitally she was stable. On Clinical examination patient had dullness and reduced breath sounds over the left infraclavicular region.
4. III.
5. Investigation
Antero-posterior and Lateral view Chest X-ray revealed a large well defined homogenousradio-opacity in the left upper and part of the mid-zone. Her CECT Chest showed a large well-defined peripherally enhancing cystic lesion noted in the left upper lobe measuring approximately 10x9.5x8.7cm (CCxTRxAP). The lesion is seen adjacent to the arch of the aorta with well-maintained fat planes; likely? Large cyst and which showed no evidence of invasion into lung parenchyma, mediastinum, or the chest wall. But lesion near to the left subclavian vessels. Pulmonary function tests revealed an obstructive lung disease.
USG guided Trucut biopsy shows linear tissue bit showing spindle cells with spindle nuclei along with few ganglion cells suggestive of Ganglioneuroma.
IV.
6. Treatment
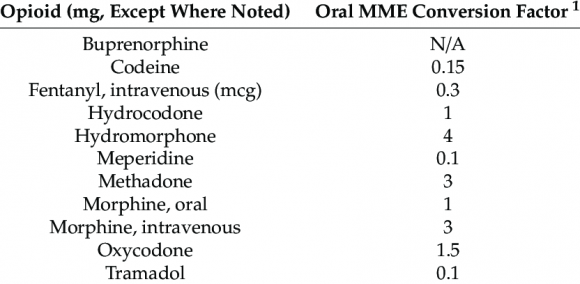
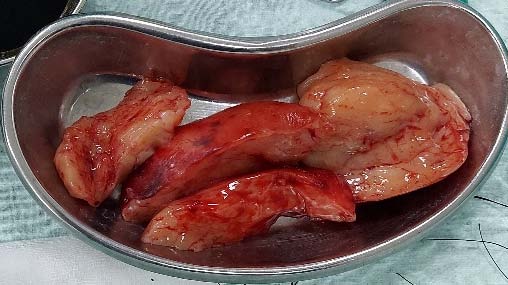
Surgery is the preferred treatment for benign tumors of the posterior mediastinum. Although these tumours are histologically benign, they can be aggressive, compressing, or invading nearby mediastinal structures. Given this potential, these tumors are resected. Ganglioneuroma has a near-zero recurrence rate, and surgical complications are uncommon. [1] Left anterolateral thoracotomy was performed with access through the fifth intercostal space. Intraoperatively there was evidence of a wellencapsulated mass, slightly adherent to upper lobe of left lung, compressing it. We identified dense adhesions between apex of the mass, and left subclavian vessels, 1 st and 2 nd rib. En-mass resection was relatively arduous, the decision was taken to carry out piecemeal excision. The mass was 12x10x8 cm in size. Mass was densely adherent to left subclavian vessels, hence had to be compromised. The Left subclavian vein was ligated. Left subclavian artery approximated with Autologous Interposition Saphenous Vein Graft. After removal of the tumor, the lung was ventilated, and expansion was observed. Two Intercostal drainage tubes were placed, one for the apex and the other for the left lung base. Excised specimen was well encapsulated and had fibrous nodule with cut sections showing whitish gelatinous tissue. On histologic examination, tumor tissue comprising of spindle cells arranged in myxoid background. Ganglion cells are found in groups and scattered, consistent with Ganglioneuroma. The postoperative course of the patient was uneventful.
V.
7. Discussion
Peripheral Ganglioneuroma is a benign, slowgrowing tumor with a well-differentiated appearance. It can appear everywhere from the base of the skull to the pelvis, but the posterior mediastinum (41.5 percent) is the most common site, followed by the retroperitoneum (37.5 percent), the adrenal gland (21 percent), and the neck (8 percent) [2] [3] Thoracic Ganglioneuromas (TGs) are generally discovered as incidental findings. Thoracic ganglioneuromas may present with symptoms due to mass effect as seen in our patient. TGs have also been reported to present with symptoms of spondylodiscitis. [4] The largest ganglioneuroma in the lungs reported is 23x10x10cm [1]. They usually do not infiltrate nearby structures; however, it has been observed that they can adhere to the vertebral bodies [9] or even involve the spinal column [5], [6], [7].
The imaging features of 14 pathologically established ganglioneuromas on CT were identified by Kato et al., who found that ganglioneuromas were often well-delineated lesions with oval or lobulated contours and showed craniocaudal longitudinal growth with low attenuation on CT. [8] On CT, our case showed a well delineated homogenous lesion with low attenuation with a postcontrast density. However, there was no calcification, fat content density, or significant enhancement.
Surgery is the definitive treatment for Thoracic Ganglioneuromas [5,9,10] Fluid shifts and sudden pulmonary edema can occur when big intrathoracic bodies are removed. After decompression of a chronically compressed lung, patients could have re-expansion pulmonary edema [11][12][13]. Surgeons must also be cautious not to disturb the sympathetic trunk, a rare condition that can cause various problems, including Harlequin syndrome [7]. [14] In our patient, the mass was densely adherent to left subclavian vessels, hence had to be compromised, which required autologous reverse saphenous vein graft and patient is recovered with relatively negligible post-operative complications [15,16] VI.
8. Conclusion
Although thoracic ganglioneuromas are rare, clinicians should be aware of them and consider them in the differential diagnosis when necessary. If thoracic ganglioneuromas grow significantly, they can induce compressive symptoms and parenchymal damage. Most of these masses are benign and complete excision of TG is usually safe and achievable. Preventing local extension, obtaining a histological diagnosis, preventing malignant transformation, and determining the need for subsequent therapy are the goals of surgical removal. [17]A combination video-thoracoscopic and neurosurgical approach is required for the dumbbell variety of neurogenic tumours with extension into the spinal canal. [5] Estimation of surgical risk factors based on radiological investigations is useful when planning TG operations. Because of the mass's proximity to the aorta, left pulmonary artery, and left subclavian vessels, a thoracotomy was the safest option because it allowed for the prompt intervention of an operating complication. Large intrathoracic masses necessitate special consideration during the postoperative period to avoid fluid shifts and hemodynamic instability [12,13]. The high mortality rate of this event necessitates careful surveillance in the postoperative phase. Surgeons must also avoid disrupting the sympathetic trunk, which can result in a variety of problems, including Harlequin syndrome, which is characterized by asymmetric sweating, and flushing on the upper thoracic region of the chest, neck and face [14]